So, finally the heart results have come back. If you haven’t been keeping up with all of my latest and greatest developments in the slow-moving train wreck that is called systemic sclerosis, let me quickly catch you up.
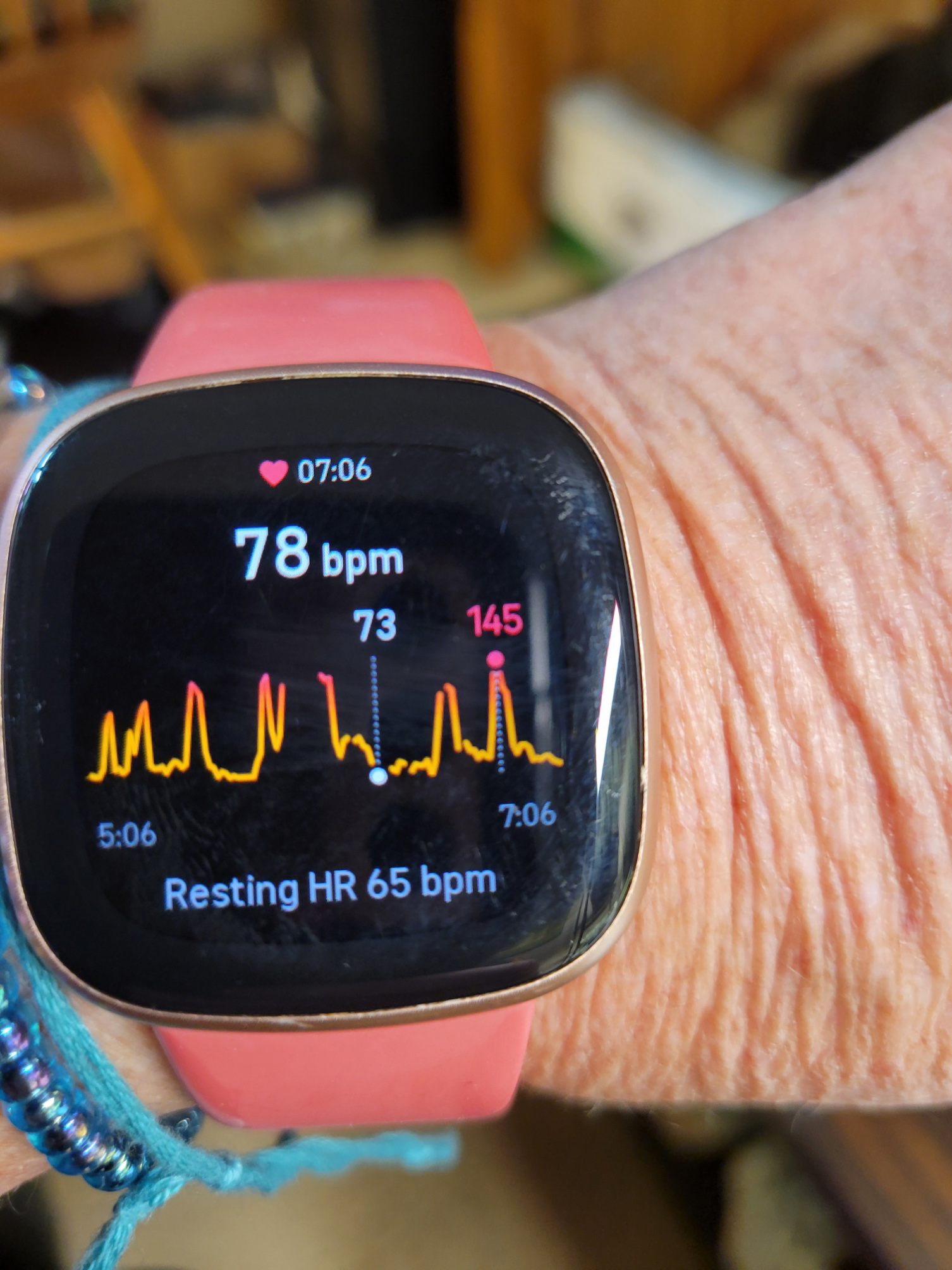
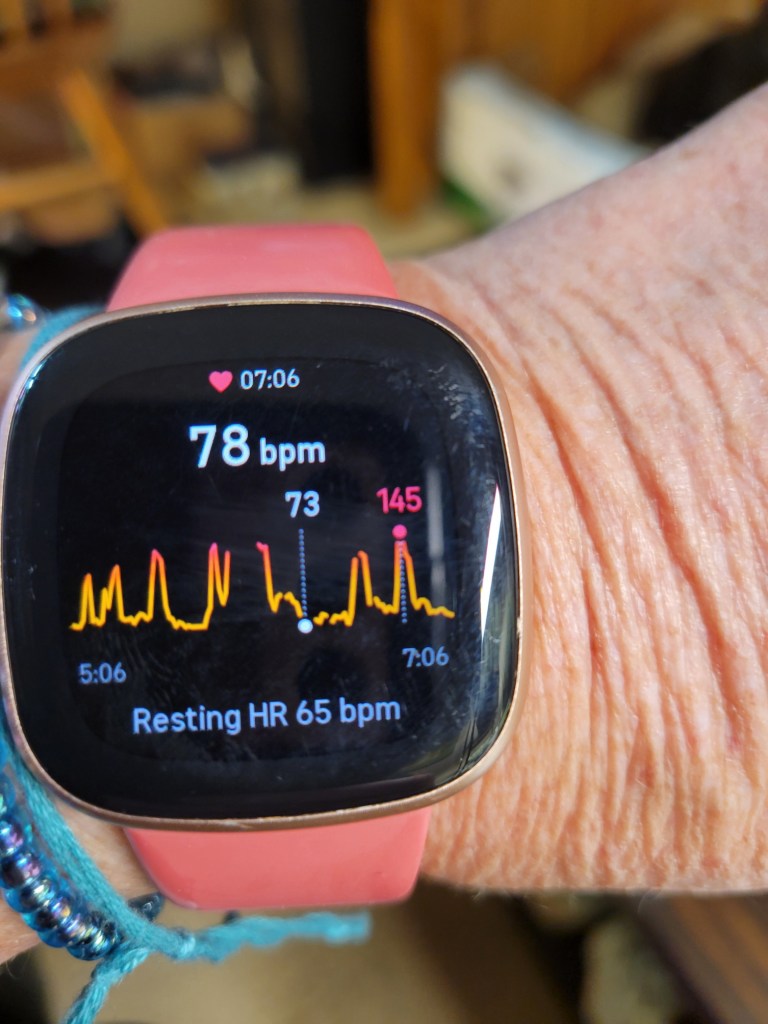
Over the summer I started to notice that my Fitbit was alarming frequently because my heartbeat was high. My heartrate was jumping suddenly from a moderate mid-70s bpm to over 140 bpm: cue the panting! I’d have to stop whatever I was doing to lean over while I caught my breath, and then it would be over. Sometimes my chest hurt, and I was pretty sure that this was contributing to my fatigue.

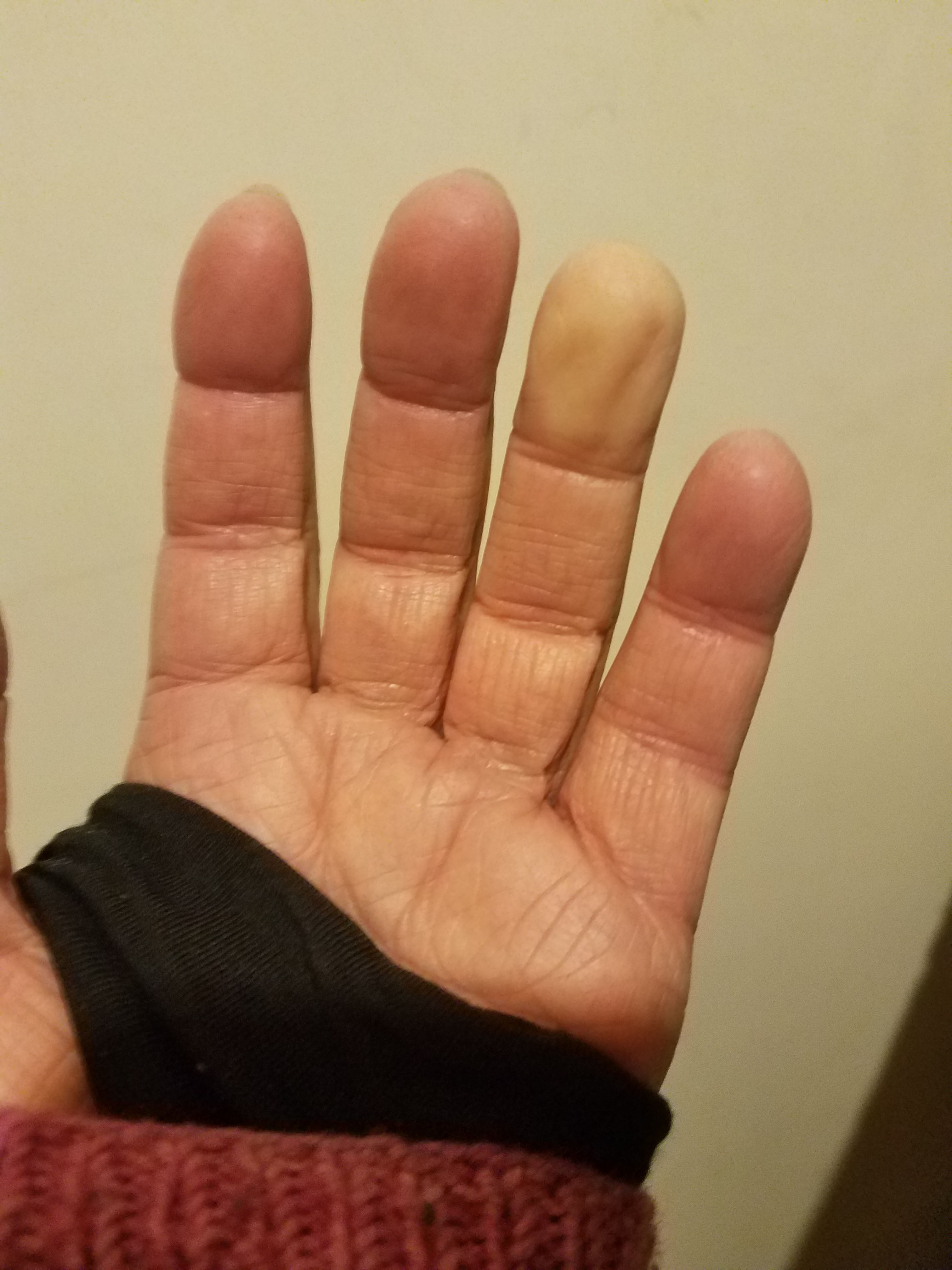
I do have a long history of shortness of breath, and I’ve been diagnosed with several heart and lung issues that explained my symptoms: pulmonary hypertension, cardiac fibrosis, fluid around my heart, lung disease, and… yeah. I’ve been short of breath like this for a long time and I’ve just been dealing with it as my new normal. Still, the Fitbit was new data, so I sent an email to my cardiologist, and he ordered up a 30-day heart monitor test.

Tuesday afternoon the results were in, and my cardiologist contacted me with the results. It’s kind of a good news/good news/bad news diagnosis. I have a type of supraventricular tachycardia called paroxysmal atrial tachycardia (called PAT for short). I had to do some google searches to understand those crazy terms. The commonsense translation would be: sudden onset rapid beating of my heart’s upper chamber (the atrium). In even more simple terms, my heart rhythm slips out of control suddenly and the upper chamber is beating waaay too fast. Here’s the good news: this is a pretty benign heart rhythm issue (no blood clots, heart attacks or strokes here!!), and it can be treated (probably). The bad news is… I’m stuck with it, and it is pretty unpredictable. The other bad news is that I should go on oxygen more often in the daytime as PAT episodes seem to be triggered when my oxygen levels drop. That’s why it hits when I’m folding laundry, or right after coming up the stairs, or when I rush to the door to answer the doorbell…

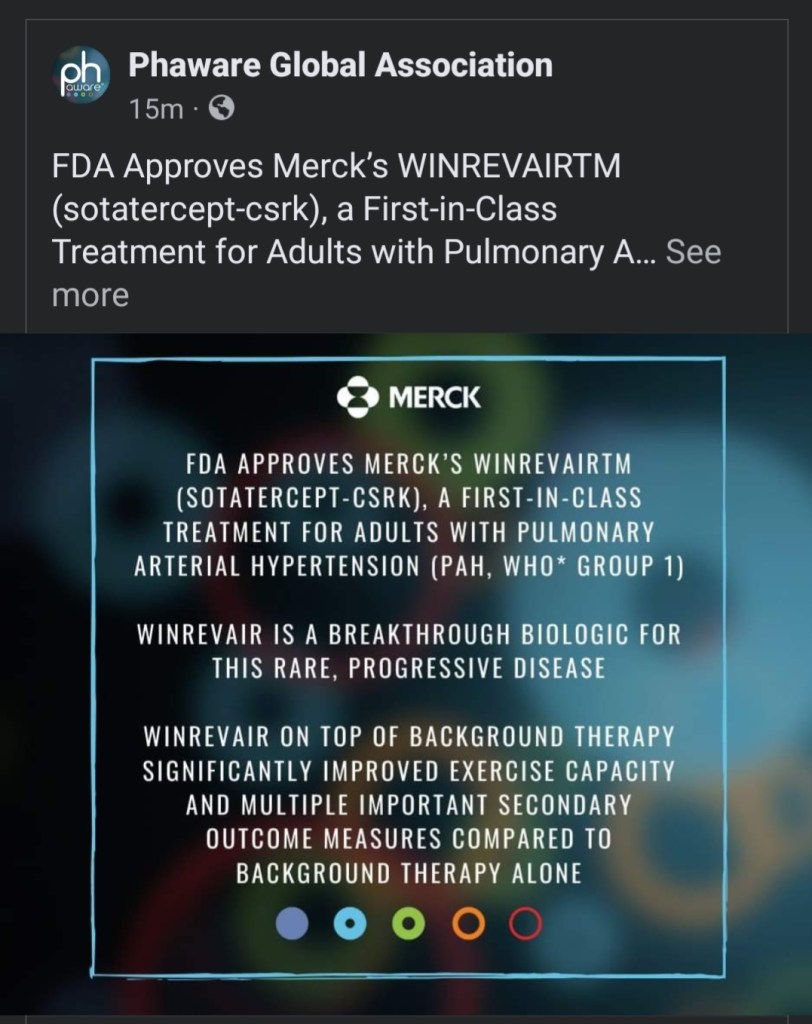
Why wait on a new drug? Well… I’m just now recovering from a pretty bad flare that hit my tendons, wrists and knees with paroxysmal fury. Paroxysmal is a great word, don’t you think? What is really crazy, my heart symptoms improved while I was down with the flare, making me wonder if the two are somehow connected. I want to wait to start a new medication until after my rheumatologist has a chance to sort out what is happening with my poor wrists and knees. I am suspicious about calcium being involved somehow, and the treatment for PAT involves calcium channel blockers. There may be no connection if there are different pathways involved, but still… calcium is the multi-headed monster of the moment with new calcium deposits appearing on my arms and legs, osteoporosis, and a previously floated notion that I might have pseudogout (which is caused by calcium pyrophosphate crystals in joints… wrists and knees being hit the worst… and my knee x-rays showed that I had calcium deposits in the tissue around my knee…). My cardiologist is okay with a delay in treatment with the understanding that I need to contact him if things get worse.
I just love my doctors!
So, here is the lesson from this adventure. Data really changes a conversation. Having that picture of my Fitbit made a huge difference; after months of explaining that I had sudden shortness of breath things changed with the one email and attached photo. The results of the heart monitor test have now returned a data-driven diagnosis that helps me understand what is happening and makes treatment possible. It is helpful to email your doctors (instead of making phone calls…) as you have a clear record of your interaction. Google with abandon!! Rely on the advice of your doctors; they went to medical school after all, but try to be an active partner in your treatment plan.
Dang. There is another diagnosis on that growing list… no one will believe me so we should just keep this quiet. Paroxysmal Atrial Tachycardia.

Postscript: I forgot to mention, that of the three types of supraventricular tachycardia, PAT is the one that is the least common. Figures. Once a zebra, always a zebra!!