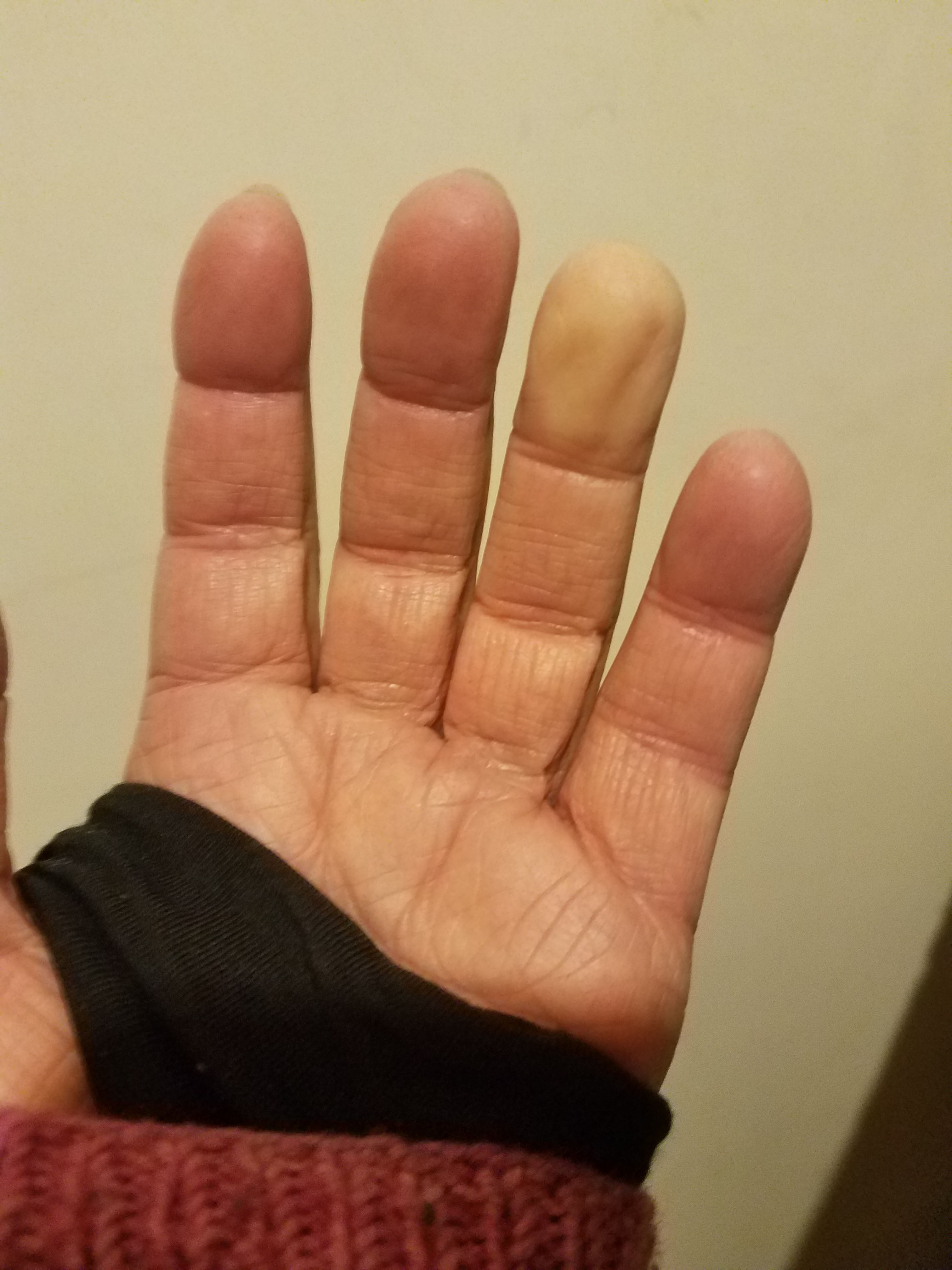
It was the third day in the Intensive Care Unit following my lung biopsy. I was sitting up in the bed, rocking all of my tubes but finally off the high flow machine, drinking a Starbucks latte and chatting with a visitor. The nurse came in the door and stopped short, taking in the scene of me, the Starbucks, and my visitor. “I don’t believe it!” she exclaimed. “They just told me all the things that are wrong with you, and I walked in here expecting to see a gravely ill person. Instead… here you are! Not what I expected!”
“Yeah, I get that all the time,” I told her. It’s the curse of chronic illnesses… you adjust and stop acting sick. Your condition is invisible, and it is too exhausting to explain to people what’s wrong when the list of diagnosed conditions is… well… exhausting. Seriously, if you say more than a couple of things it starts to sound like you’re just making things up. It doesn’t help when the diagnoses sound fake to begin with (systemic sclerosis associated interstitial lung disease… it’s called SSc-ILD for short, but still… sounds like something invented in a science fiction novel, right?). It invariably gets worse if people start to share back some rheumatic or autoimmune conditions that they know of (like fibromyalgia or Raynaud’s), and you are compelled to say… “Oh, I have that too…” See what I mean? Attention-seeking hypochondriac is sure to cross their minds. I mean, I would wonder that… It is much easier to cover up as much as you can and act normal.
I’ve been thinking about this a lot. Several patients in the support groups that I belong to have been struggling with family and friends who are unable/unwilling to accept the diagnosis. They don’t want to hear about it, they don’t want their lives to change, and there is no support. There has been heartbreak and tears, to be frank. Others in the groups have shared that their families also refuse to accept the seriousness of their condition(s) because there have been years of struggle to obtain the diagnosis, and after so many doctors have said that it’s all in your head, or, you need to control stress better, they kind of believe that. From the perspective of these family members, their scleroderma family member is just trying to milk the diagnosis for attention. To make it worse, some patients (and this is exhausting, believe me) start to list all of their symptoms as if to justify their diagnosis. It is a little desperate, and more than a little heartbreaking.

Then there is the more insidious problem: what did you do to make this happen? I have been asked that, and it usually is followed by advice about things that I can do to control my scleroderma and the resulting lung/heart complications or even how to make myself get well. The implication is, if you don’t do this (herbal treatment, sunshine, exercise, wacky stem cell injection), it is your own fault that you are sick!! It happens to a lot of us. It eats away at self-confidence, and makes me, and other patients question just how sick they really are.
I, and a lot of others in my extended scleroderma community, feel like fakes a lot of the time. Like, almost all the time!
I mentioned that to my pulmonologist last week on the phone, and he was really direct in his response: do not fall prey to imposter syndrome!!! This is really happening to you, you are dealing with it very well, but you need to remember to take care of yourself!

I had never thought of imposter syndrome in this way, but I think that his point is well made. Maybe I should have a poster made with this written on it. With some sunflowers and a tuxedo cat for interest. Every person diagnosed with a serious chronic condition needs this, because it is easy to just trick yourself into pretending that you are “better” and then the bad decisions get made. Like going off your meds. Or partying like it is 1999. Or eating all of those things that are essentially forbidden at once! There has been a rash of wailing patients in my online support groups who say things like… I went off my meds and started treating myself with natural remedies, and now [insert new symptom that has them terrified] is happening. Yep. That is imposter syndrome, hard at work. No wonder my doctor was so firm with me.
Because the point that he was making is that I am pretty ill, and I need to own it. I’m in a very small group of scleroderma patients who have the full battery of the more serious systemic sclerosis complications: pulmonary hypertension, interstitial lung disease, and diastolic dysfunction. I am being treated aggressively for those conditions, and I am doing really well, but they haven’t gone away.
I finally pulled myself together to check what the survival rates are for patients with two of my concurrent conditions (SSc-ILD-PH) and discovered that there are recent studies that looked at patients being treated with the same drugs that I am on.
- This study, done in 2009 with patients on the same drug regimen as mine, showed the 3-year survival rate to be 39%. Oh, oh. Not an imposter any more.
- This study, published in 2011 has a 3-year survival rate of 47%. Oh. That’s better.
- A huge study done in Germany and published this year, shows that scleroderma patients with ILD-PH had the worst outcomes: the 5-year survival rate was 79%. Gosh, that is a good-looking number!
I see a trend. Do you see a trend? It looks like things are getting better and that survival rates are going up. I have to admit, when I saw that first 39% I almost panicked and stopped searching, because… I was diagnosed and started treatment for pulmonary hypertension and diastolic dysfunction exactly 3 years ago. The ILD diagnosis came in a few months later. The clock is ticking, and I am one of the 39%… talk about imposter syndrome: how can I be this functional when the majority of patients like me are already dead?? I’m a fake, an imposter!! That can’t be true, it is not true, and that new data shows what is happening: it looks like the treatment plans of today are really making a difference. My pulmonologist feels that the drug that I’m taking to control my lung disease is a game changer, and that drug was only approved for use with scleroderma patients within the last decade.
For some reason the term 39% Imposter has stuck with me. That’s me. I’m not really all that sick, because only 39% of me is pretending to be sick. Or well. Whatever works today. I’m thinking about a tee shirt with the slogan. I’m rocking the imposter persona. Maybe a shirt that says 39% Imposter and 100% Survivor…
I mailed back the heart monitor last Monday and now I’m waiting for the results. It has been a difficult three weeks because the flare just won’t go away, my wrists and knees are being bad boys, and now I have painful heart palpitations. Sigh. It is always one thing after another.
And yet, in my heart, I don’t feel sick at all.
Imposter Syndrome.
But only 39%.