
The BLZ has been waiting a long time for this…
Five years ago I came down with the flu and ended up in Urgent Care struggling to breathe. I scored some antibiotics, steroids, and cough medicine. To fight the virus I was told to go off my immunosuppressant drugs for a few weeks until I got better, stay in bed, and load up on chicken soup: it took a couple of months but eventually I got back on my meds. Except… things weren’t quite right. I panted for air every time I came up the stairs and I noticed that my lips were turning blue. My blood pressure was too low and I had to stop taking my hypertension medicine. I felt dizzy and light headed sometimes.
I was a newly diagnosed systemic sclerosis patient and my doctors began running tests to see if my disease was impacting my lungs. Nope. Not my lungs. Tests were run to see if scleroderma was attacking my heart. Nope: my heart seemed to be normal. There were some anomalies, but my doctors decided to just monitor me through routine testing and see if things changed down the road. My red blood cell counts were way too high, and I had nocturnal hypoxia, so I was started on overnight oxygen. I was tested for various conditions that could account for the weird test results, but I always had a normal result.
I struggled on, battling for more testing, as my doctors kept reassuring me that I was okay. Hey, I had a blue face and panted for air when I climbed stairs; vacuuming could put me on the floor. How could this be “normal”? Ugh. Welcome to scleroderma, I thought.
I began to think of myself as the Blue-Lipped Zebra (BLZ). If I didn’t have a rare disease confusing the issue I would be getting better health care, it seemed. If doctors didn’t tend to apply most-common-cause thinking to my condition they might get to the bottom of things faster. It was, in my mind, a huge complicated mess as my doctors applied best practice (and rigid) diagnostic parameters to my symptoms or zeroed in on specific complications of my scleroderma and ignored other possible (and to be fair, rare) causes for my symptoms. I worried that my doctors had just parked me in a holding pattern as I slowly got worse; it is hard to advocate for yourself when you are sick and dependent on your doctors for help, even if you think that they are dismissive and borderline disparaging.
I struggled on as my face became more blue, my red blood cell count higher, my panting for air more common, and the occasional near-fainting event left me collapsed on the floor. I began to ask for a right heart catherization procedure to directly measure the pressure in the right side of my heart. “Oh. You don’t want that,” I was told. “That is really invasive testing.” Umm… I think I do, I would reply. Nope. Nope, nope, nope!! “Not even on the table,” one pulmonologist said.
During lockdown last year I got much worse; ironically lockdown also gave me the opportunity to reboot, fire my old doctors and acquire new ones. My new team of doctors this spring ordered up testing that showed definite issues with my heart and lungs. I am now a heart failure patient (the wall of my left ventricle are too stiff and scarred to beat well) and there were concerning findings that suggested that I had developed pulmonary arterial hypertension (PAH): there are areas of cell death in my lungs and my pulmonary artery is too big. There is too much fluid around my heart, a suggestion of ongoing inflammation. I have a hole in my heart between the atriums (a cardiac shunt) that is impacting blood flow. I was gently prepared for the PAH diagnosis, assured that there were great drugs that could help me, and a right heart catherization was ordered by my new cardiologist.
Yay!! About time!!!
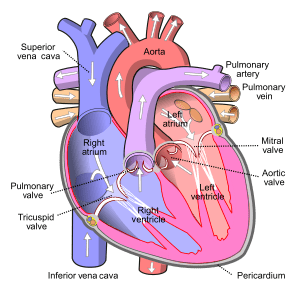
Finally, after 5 years of struggle, I was yesterday wheeled into a procedure room to a waiting team of specialists who hooked me up to equipment and took me though testing to get a better look at my heart: I learned in recovery that this team calls themselves “the pit crew”, and that is exactly what it was like. Within 5 minutes I had completed a breathing test, was on oxygen, wired up to a heart monitor, hooked up to an IV, medicated, prepared with surgical drapes, and swathed in warm blankets with a heater by my feet. There was music playing and the crew was cracking jokes as they darted in and out from the table getting me ready. I was knocked out for the echocardiogram imaging of the back of my heart that was done using a probe in my esophagus, but they woke me up for the main event: the right heart catherization. My cardiologist inserted a probe into the carotid vein in my neck and threaded it into my heart by way of the superior vena cava (blue side of the heart diagram above). People, this was the most amazing experience ever! There was a huge screen showing the progress of the probe and I could watch and ask questions as the line snaked through my heart; there was absolutely no pain. “Well, this is interesting,” said my cardiologist at one point, and there were more measurements happening and a flurry of new activity from the team. The BLZ felt a surge of elation: they had found something, and it was NOT what they expected.
Back in recovery my cardiologist caught up with me again. I had done great, he said, and he just beamed as he told me that I absolutely did not have PAH. This is great news, he assured me, great news!! There is another circulation problem in the lower part of my heart, between the ventricles. There is blood coming in from the left side of my heart and mixing with the blood on the right, disrupting the flow through the heart and robbing me of oxygen to my body. I have a second, more serious, cardiac shunt, and now it is a question of locating that pesky little guy and doing something to fix the problem.
It has been FIVE YEARS, people. If I hadn’t had my trip into the cath lab yesterday my doctors would still be nagging me to get more exercise (the BLZ just barks in laughter), offering me antidepressants, or insisting that I must have sleep apnea. I feel so validated!
My cardiologist is now going over my previous imaging to find the hole now that he knows what to look for. I was told that I may need to go through more testing to definitively characterize the opening, but this is huge forward progress. I suspect that I am facing open heart surgery down the road, but I am elated that the progressive and eventually fatal diagnosis of PAH is now off the table. Things are looking up since my heart failure will now be much easier to treat.

Today I am waiting to hear back from my cardiologist who is going to email me with follow up instructions after he has finished going through the data and past test results. I’m on oxygen, knitting, and feeling pretty calm about all the new developments.
Almost exactly 7 years ago (August 28th was the anniversary day) I was diagnosed with Limited Systemic Sclerosis and Sjogren’s Disease. I have learned a lot along the way, but the best, most important lessons have been about self-advocacy, facing down the worst case scenarios, communicating with your doctors, and maintaining a good attitude.
Yesterday this all paid off for me big time.
Note: The fabulous BLZ graphic was made for me by my exceptionally knitworthy niece Melissa and her beautiful and talented daughter Eleanor.



FAR OUT, Marilyn !! How lucky you are that you actually grasp all that medical terminology so that we can (almost) grasp it too ..
I wonder how many ill people there are suffering needlessly because of incompetent medical ‘care’ ? – more than one or two, I fear. So happy that you clutched the nettle and pissed them right off, turning your state of health around. You have done this, even though you’re still not without health issues; and you’ve done it because you believe in yourself. BRAVO !! – BRAVO !!!!!!
I am lucky: very, very lucky. I have a biology degree and spent years acquiring essential background knowledge through various career adventures that are now coming into play. Of course, I spend a lot of time talking to Dr. Google about a lot of this as I try to learn enough to understand what my doctors are telling me.
I suspect that most people are okay with their medical treatment, but those of us who are at the far ends of the bell curve because our conditions are rare it is really hard. I finally have started call out some of the things that are said to me as “medical gaslighting” because it is so egregious. Doctors will calmly tell me that what I experienced really didn’t happen and that my condition is actually _____. (fill in the blank) I’m always so blindsided that I can’t respond as well as I should, but it helps to acquire all of the test results, go over them with my PCP, and then spend time with Dr. Google reading up on body parts. Whew. It is a lot of work playing medical vocabulary catch-up.
I know a lot of people don’t want to hear bad news and insist on being positive no matter what, but I think that is not productive. It is always better to know the diagnosis that is being considered, understanding what type of treatment and prognosis is associated with it, and then making informed decisions based on that knowledge. It is better to know then to worry about nebulous possibilities; and in this case it helped me press for the testing that I needed to get the help that I need.
Indeed .. I suppose your earlier academic work has enabled your ever-expanding PKB on matters medical. Keep it up, my girl ! 😀
Thank you so much for sharing your journey. While my health problems are not quite where yours are, there are moments where this gets quite scary…and then you wonder if docs are capable of empathy while they dissect your life (but like that bio student destined to be a garbageman). I’m glad you got a team of docs that work with you. Here’s hoping it continues, for both of us!
Hugs to you, I know how difficult it is to deal with ongoing health problems that are hard to quantitate medically, and how soul draining it can be to interact with dismissive doctors who don’t emphasize. I cried all the way home from the first cardiologist appointment, but in time I navigated the system to get a new cardiologist and this is the outcome. Hang in there; I hope that you are able to get to a better place soon.
What a fabulous outcome to your day, mentally and physically. To be believed, to be proved right. I’d be sending those old doctors a “I effing told you so” message. Onwards and upwards though, now it’s properly diagnosed progress should follow. Well done for persevering.
Oh my gosh, you never saw a person more excited about a cardiac shunt than I was once I got the news. My doctor was so happy and I was even more so. I do wish I could send my old doctors some flaming Howler mail by messenger owl. This took so long because they just kept dismissing my claims based on the test results they had. My new doctors are of the mentality that if the first round of testing doesn’t show anything there needs to be more tests: they accept my symptoms as valid. Yay! That seems to be reasonable to me. 🙂
I am so happy for you! It’s crazy how hard you have to work, as a patient, to get some doctors to listen.
Now armed with answers, you can make a plan and put it into action. It has to be such a relief.
The rest will be easy by comparison. It seems like an odd thing to say about your cardiac issues but believe me, any treatment or surgery will be a cake walk compared to the struggle you went through to get an answer.
I know. I am all like… yippee! surgery!! I can handle surgery, no problem!!! I will be able to actually walk to my front door without putting my head down and panting for a little bit before I open the door… I know that this isn’t going to be a cake walk, but there finally is going to be a plan.
You are right…it will be magical for you to be able to walk to your door and breathe normally. I’ve had 5 surgeries and 2 outpatient surgical procedures. I have cried tears of joy each time my health moved one step closer to “normal.”
Thank you so much for that. Hugs to you, I hope that things keep on improving for you.
Congratulations on your good sense and determination. And your knowledge and ability to use it.
Thank you. I also think that I finally got some good luck, too.
Well, yes
Hooray a result at last!
I’m so glad the doctors finally arrived at a real understanding of your condition! This should lead to treatment that helps!
That’s the hope!
I’m so pleased your new doctors are actually doing their job! I love the blue lipped zebra graphic!
I am too! I think that the big difference is…1) all of my doctors are now young (under 40) and 2) they are attached to a major teaching hospital associated. The hospital where I had the catherization test done is one with a highly regarded cardiac team and there were two trainees in the room during my testing.
I love that graphic too! My niece sketched it our and her daughter produced it. She is so talented!!
I’m SO glad they are finally getting to the bottom of this. I will be praying for this.
Thank you. What a relief to finally get a solid indication of a problem that explains all of my symptoms.
I am so happy for you (well not happy for open heart surgery and what you are dealing with); honestly why does it take such super human pushiness on the part of patients to get doctors to actually listen to them? I’m in the process of firing my current pulmonologist and seeing a new one with more of a focus on inflammation and arthritis induced lung inflammation as being more of causing the problem than only asthma or sleep apnea. He’s applying what he knows on what he sees and not thinking outside of the box like one of my other doctors is thinking. I so wish you well and am so happy you will be getting the appropriate treatment you actually need. Thank you for updating us!!! Take care of yourself
I had to fire a pulmonologist, too. I think that she was really okay for treating asthma, but I’m a lot more complicated then that and inflammation is a huge part of my problem. She was one of those people who kind of attacked me in her office which I view as a strategy for putting patients on the defensive so that they don’t make demands. My face literally turned blue while I was talking to her in the exam room and she just said… hum… must be something circulatory because it isn’t your lungs… if only she had made a referral based on that observation it would have been much better for me the LAST THREE YEARS!! Whew. Anyway, I do hope that you find a doctor that you feel comfortable with and in whom you can feel confidence.
So incredibly frustrating for you and soooo incredibly dangerous.
Well interestingly two asthma doctors keep saying it’s not asthma and the one who has known my lungs for 15 years and was troubled when her testing started showing issues believes it’s inflammation from the arthritis (and of course aggravated by long covid, which is inflammation). I hadn’t seen her for awhile and consulted with her recently, she suggested a biologic may help me more. Anyway, would explain why a lot of the asthma drugs don’t help. Except prednisone always helps. I’ve had asthma for 40 years and that was always reversible. So we shall see!
Your blog has certainly helped me so much, hang in there, and please keep us posted. Many prayers and virtual hugs to you.
I have struggled and struggled with inflammation related issues for years while doctors either offered antidepressants or told me it was asthma. This is crazy, but I am doing so much better this year with no brain fog, less pain in muscles, and breathing better. I am not sure what exactly caused the improvement, but I am riding the wave! (a lot of things changed this spring like getting the Covid vaccine, a steroid injection in my hip, stopping one of my drugs, etc. I’ll never figure out which one made a difference…) I started taking some anti-inflammation supplements (tart cherry, curcumin, krill oil) and started using over the counter Voltaren on my worst joints. I had noticed that I could buy myself a couple of good days if I took ibuprofen or my inhaled steroids which made me decide that this was inflammation. I highly recommend keeping a journal or food log to help you sort out what hurts and what helps. It is so frustrating to get on top of things, and having long Covid certainly isn’t helping things!! Have you gotten the vaccine? Some long covid patients are saying that their symptoms improved. Ask how that biologic works… I would kill for one that could help me but there isn’t one. I find them appealing since they are more like the highly-targeted cruise missile treatment option as opposed to the carpet bombing options that are being used with my condition like chemo or immunosuppressants.
Hugs!! I hope that you aren’t getting a lot of wildfire smoke these days… a wave of smoke is on its way to us and I’m not too excited about it! Talk about inflammation…
I am so glad you got some results and progress on your condition finally! Yay for your new team of doctors and double extra YAY for your persistence and courage to keep fighting!
Thank you! I still am feeling pretty darn good about finally getting an actual result that explains my blue face!! Vindication!!
I am very happy that you found doctors who were willing to listen to you and test you with open minds. My experience is that doctors have their strengths and weaknesses and get stuck in ruts like everyone else.
I’m glad that it has all worked out. I agree that, just like everyone else, doctors come with all versions of problem solving techniques. Now that the heart problem has been identified I realize that many of the symptoms that I kept reporting were actually due to my ongoing oxygen shortage; if only they had taken me seriously sooner and not chalked me up as a “complainer” I might have gotten help sooner, but to be fair, when you are an outlier what you are telling the doctors just doesn’t seem reasonable. The big difference that I made was to transfer to doctors all associated (within the Kaiser system) with a teaching hospital. Huge improvement, but it also may be do to their exposure to more ideas and unusual patients. I do have to say, doctors in ruts are much more likely to offer antidepressants to their patients who are struggling. What is up with that?!!
Hi! Thank you for sharing, and like the others, I’m glad you found a care team willing to listen. I wanted to mention, I work with an organization called Savvy Cooperative. We’re currently seeking diastolic heart failure patients and their caregivers for a virtual round table to hear about the patient and caregiver experience. Please let me know if you’d be interested! You will be compensated for your time.
I don’t think that I would meet your patient criteria since my caretaker is a cat (!) and my medical situation is pretty complicated at the moment. I am a heart failure patient, but at the moment that is the least of anyone’s concerns as my doctors are still chasing down the cause of my symptoms and I’m going through a lot of medical testing at this time.
I understand. I wish you the best in your journey!