Last Monday, May 2nd, was the date of my lung biopsy procedure. My pulmonologist had diagnosed me with interstitial lung disease a couple of months ago and the biopsy was required to definitively diagnose the type of ILD I had. This is kind of complicated, but the simple reason for the biopsy is that I don’t really fit the profile of the usual scleroderma ILD patient, and the treatment is expensive and somewhat risky. Biopsy time.
At 4:30am Monday morning my son drove me through the rainy dark to the hospital where I was going to be admitted for the surgery. I had on my new raspberry clogs for good luck, and I was exhausted after being up most of the night completing pre-op tasks at home. I was fighting off a sense of impending disaster…

The day I met with the surgeon he drew a funky little drawing on his white board to explain what he was going to do. Check out the diagram above: your right lung is actually different from the left with more tissue and three lobes. My surgeon planned to use special instruments guided by a tiny video camera (VATS) to go through my chest wall and get the tissue samples. This is a minimally invasive procedure that will only take a few minutes. The catch: the right lung will be deflated before he takes the samples.
Atelectasis is the medical term for a collapsed lung. Both of my lungs were experiencing incomplete atelectasis at the time of my last CT scan, and I’d been getting steadily worse all April. I was a little concerned, but I trusted that all would work out fine in the end. I was prepped, bundled up, and rolled off to surgery. There was the most fantastical robotic surgery machine in there, but before I even got a great look at it, I was on the table, a mask was put over my face and I was gone…
… and I emerged from unconsciousness at the bottom of a rugby scrum with all these faces looking down at me. I was in pain, a lot of pain, and I couldn’t breathe at all. The muscles on the right side of my back were seized up and cramped in what felt like Charlie horses, and I was thrashing around as I tried to get someone to rub on my back muscles. The rugby players in masks (I was later told that there were 8 of them) were attempting to hold me down as they put hot packs under my back, removed my oxygen cannula, and placed a larger oxygen mask over my face. “Do you remember the Xray?” one of them asked. Oh. That’s what set off the muscle cramps. My oxygen was below 75% even on highest oxygen flow available in the recovery room. I got transferred to the ICU.
That right lung refused to reinflate. I couldn’t be given any pain medications or fluids until my oxygen levels came up. New doctors began to arrive and talked to me. To be clear, talking set off coughing and was very painful. I just wanted someone to help me, not talk to me! A pulmonologist arrived to doctorsplain my disease to me and informed me that he was changing some of the drugs used to treat my lung and heart conditions. I told him that I didn’t know him, he couldn’t make any changes to my treatment plan without talking to my doctors, and that I needed him to do something right away to handle my immediate situation (I was in acute respiratory failure). He argued about contacting my doctors. I insisted.
I think that I deserve a huge gold star for standing up for myself while in extremis.
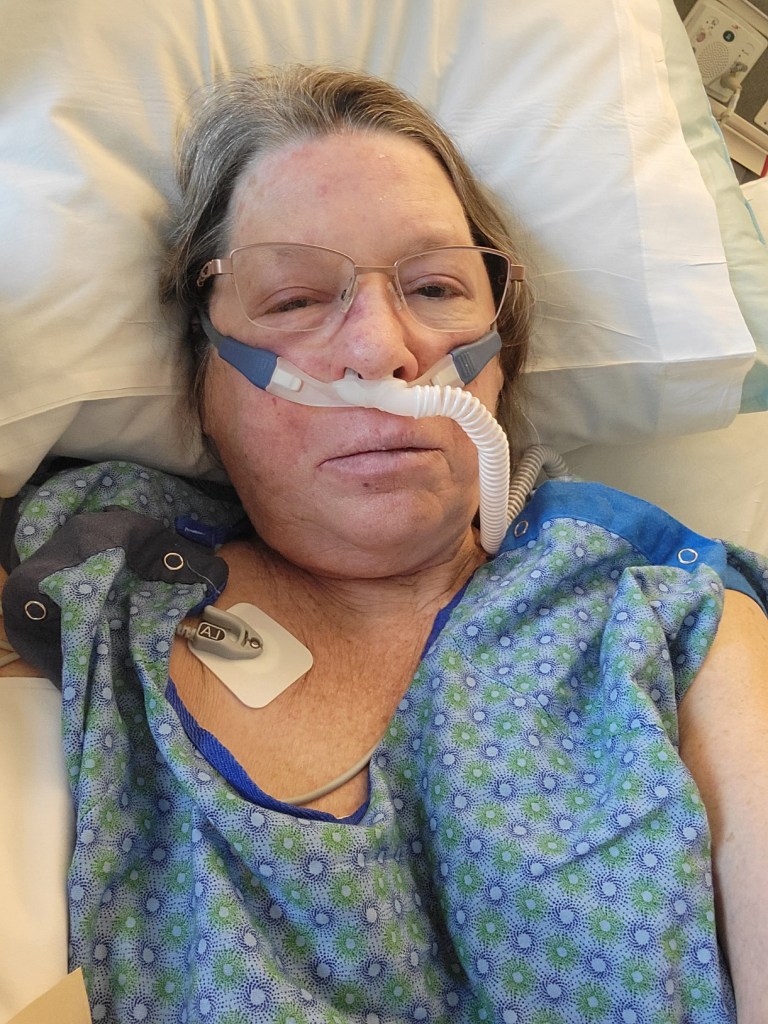
I kind of look like I was underneath a rugby scrum, huh. That machine delivers heated water vapor and oxygen at the unbelievable rate of 60 liters/minutes. My oxygen came up into the low 90s on the machine and I finally received oxycodone. Yay!!! The last oxygen number on the monitor before I fell asleep was 94%.
The next day they got me up into a chair (more oxycodone!) and I started respiratory therapy to get the lung working again. On Wednesday my chest tube came out and during the day the flow rate on the machine was reduced until I could come off it.

That annoying pulmonologist came by every single day that I was in the ICU; my doctors had called him back! After talking to them he made some med changes (and told me that it a shared decision) and his manner completely transformed. The physician’s assistant who removed my chest tube told me that she had also read the care notes with all the data, email traffic, and decision-making by my rheumatologist/pulmonologist/cardiologist team. She was struck by the interdisciplinary care that I was receiving and seemed a little wistful and envious.
Another gold star for the team!!
Over the next two days I was slowly titrated down on my oxygen while doing my lung expanding exercises without fail. Late in the morning on Friday I finally escaped.
I put on my raspberry clogs, black leggings, a little black top, and my raspberry-colored down vest. “How cute you are!” exclaimed the nurse. My son drove me home through the late morning light along streets lined with newly leafed trees. While I was in the ICU the world had turned green.
No matter how lifeless and barren things seem over the winter, spring always comes with the promise of fresh starts and new life. I still trust that all will work out fine in the end.

Now we just have to wait for the biopsy results.
